Thursday, 29th August 2019
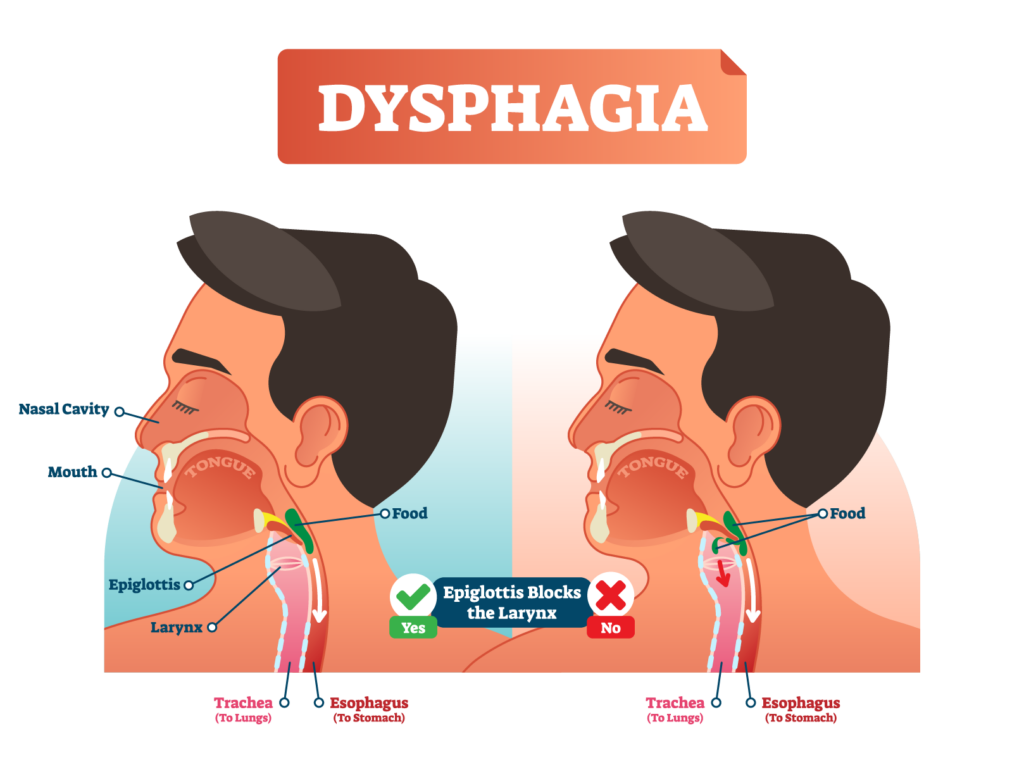
Difficulty swallowing, called dysphagia, can happen at any stage of Parkinson disease. Signs and symptoms can range from mild to severe and may include: difficulty swallowing certain foods or liquids, coughing or throat clearing during or after eating/drinking, and feeling as if food is getting stuck. As the disease progresses, swallowing can become severely compromised and food/liquid can get into the lungs, causing aspiration pneumonia.
To evaluate swallowing problems, doctors may order a test that takes x-rays while you swallow foods and liquids of different consistencies. This test shows where the swallowing problems are (the mouth or throat) and whether foods and liquids are going into the airway instead of the stomach.
Some of the signs of dysphagia are:
Strategies to overcome swallowing problems include:
The way you sit, the foods you eat, and how you eat can affect your ability to swallow. To use your posture to make chewing and swallowing easier, you can:
A person with dysphagia is at risk of weight loss, malnutrition and dehydration and should seek assistance.
Several health professionals can assist with Dysphagia symptoms including your GP, Neurologist, Speech Pathologist, Occupational Therapist and Physiotherapist. A speech pathologist can provide recommendations for swallowing management and may teach exercises, strategies and techniques for safe and optimal chewing and swallowing, specific to individual needs. A physiotherapist can assist with finding solutions for postural issues and an occupational therapist can assist with seating recommendations for mealtime, aids and equipment and techniques for using cutlery.
Drooling, along with speech and swallowing issues, is included among non-movement symptoms even though the root cause is motor: decreased coordination, slowness of movement (bradykinesia) and rigidity of the muscles of the mouth and throat.
People with Parkinson’s swallow less often, so saliva builds up and can lead to drooling. This can be embarrassing and limit the desire to go out in public with friends and family.
When severe, drooling is an indicator of more serious difficulty with swallowing (also known as dysphagia), which can cause the person to choke on food and liquids and can even lead to aspiration pneumonia.
Treatments may involve behavioural strategies and medications. Behavioural strategies include using sugar-free hard candy to stimulate swallowing and reminding yourself to keep your chin up and lips closed. The latter can be challenging, especially in advancing Parkinson’s, when the head and chin may tilt forward and the mouth may automatically open at rest. Physical and occupational therapy may help with postural issues, such as the neck and shoulder stooping forward, which can worsen drooling.
Tips to help with drooling
Speech and swallowing problems can significantly impact the lives of people with Parkinson’s and their care partners. Better treatments are urgently needed. Researchers are testing varied therapies, including new technologies, exercises and non-invasive brain stimulation, to ease speech and swallowing changes.